This is the first article in our series on stakeholder management in healthcare: What is a stakeholder exactly? Who are the most important ones in healthcare? and: How to conduct a simple stakeholder analysis?
Download the full report on stakeholder management in healthcare here– It’s FREE.
Knowing ánd working with your stakeholders is an essential skill for any project manager in healthcare. After all, your idea or your product may be excellent, if you have a poor (or none whatsoever!) relationship with your stakeholders, a lot of energy is wasted and success will not follow.
What are stakeholders?
Let's start with the basics. A 'stakeholder' is generally defined as 'any person or organisation having an interest in the implementation, financing or outcome of a product or process by another party'.
Or: groups that can be influenced by your project and/or can influence it themselves, both positively and negatively.
Primary stakeholders are directly influenced by your innovation and can also have a major impact on your project. Secondary stakeholders have no direct interest, but do have influence.
Download the report ‘Important for every new project in healthcare: know your stakeholders’
Internal and external stakeholders
This, of course, makes the group of stakeholders ánd their positions very extensive.
They are both internal (colleagues, management) and external (customers, interest groups, government, …) and the positions can even differ within one and the same organisation.
For example, GP’s and specialists might be united in one professional organisation, but their positions might differ regarding certain topics. Or: the leadership of an organisation may be convinced of a change, but the employees are not yet willing to go along with it (and vice versa).
External relations are by far the most important for innovation management in healthcare: they will mainly determine whether, how and at what speed your novel idea/innovation is introduced in the healthcare system.
The 4 P’s
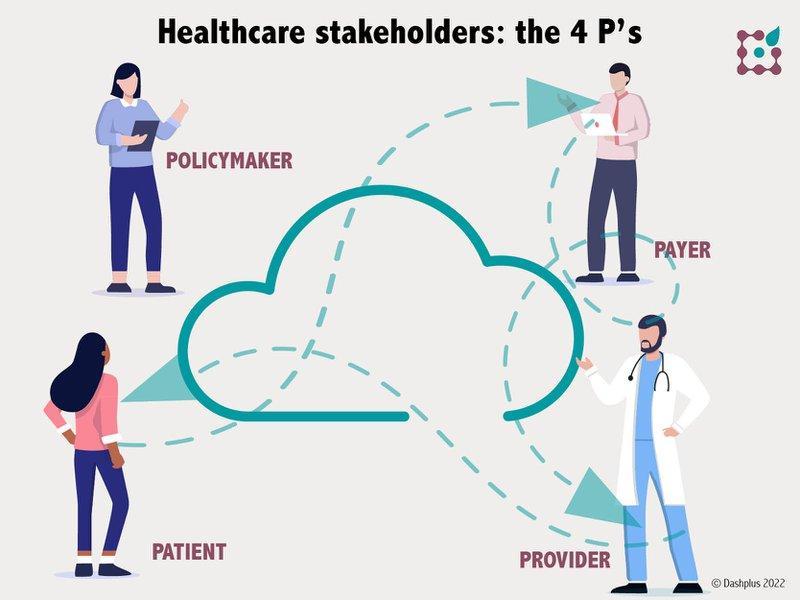
Roughly speaking, we can identify four types of stakeholders in the healthcare (eco)system: patients, providers, payors and policymakers. They all have a different role in the healthcare value chain, which means that different interests and/or visions will also play a role. But they are all connected and influence one another.
- Patients: are, basically, the most important stakeholders. They include all of us, as users of healthcare. Patients are also taxpayers and contribute to social security, and patients are voters.
- Policymakers: they define the framework within which healthcare is delivered to the citizens (patients): who can receive healthcare? Who can provide healthcare and how is it publicly funded? How do we ensure sufficient accessibility and quality? Depending on the type of the public health system (Bismarck, Beveridge or an intermediate form), the main policy makers are: the Minister(s) of Health, the Healthcare administration and a consultative structure such as the NIHDI-INAMI in Belgium. In federal states, policy makers can be either regional or national.
- Payers: they financially implement the policy rules. They provide public or private reimbursement for health services and products to patients. They also develop their own services. Public payers share responsibility for the financial stability of the public health system. Typically, they are mutualities and private insurance companies.
- Providers: they are the (para-)medical professionals delivering healthcare services. They work in their own practice or as a member of staff. We also refer to healthcare organisations as providers.
- Join our Community
There is a connection between all four types of stakeholders
Patients are often the lever for new applications. For example in digital health: patients started using innovative solutions long before payors and politicians give it further structure and support. The latter is needed to scale up and make new services accessible to as many people as possible. But it also works the other way round: in some European countries we have really seen governments creating change. This way they create opportunities for startups and new type healthcare providers. They do so by legal reassurance and/or financial stimulation. Think about the example of Portugal, France and Finland regarding digital health or Australia regarding lifestyle medicine.
Moreover, the connections between the stakeholders are changing too and new partnerships are build. Santilli and Vogenberg (2015) refer to patients as consumers and the growth of quality-measurements as some of the trends impacting HC stakeholder relations. For example, pharmacists in the US have been working much more closely with payors in recent years. Medical device companies cooperate with clinical trial centers.
In the post-pandemic area, accessibility of healthcare, scarcity of HC workforce and ‘green healthcare’ will be the most important changemakers for stakeholders in health.
Know your stakeholders
Starting stakeholder management for your healthcare project means knowing your stakeholders in the first place: who are they and how important are they for your project? This is what is called stakeholder analysis or stakeholder mapping. You make it because you will have to interact differently with each stakeholder.
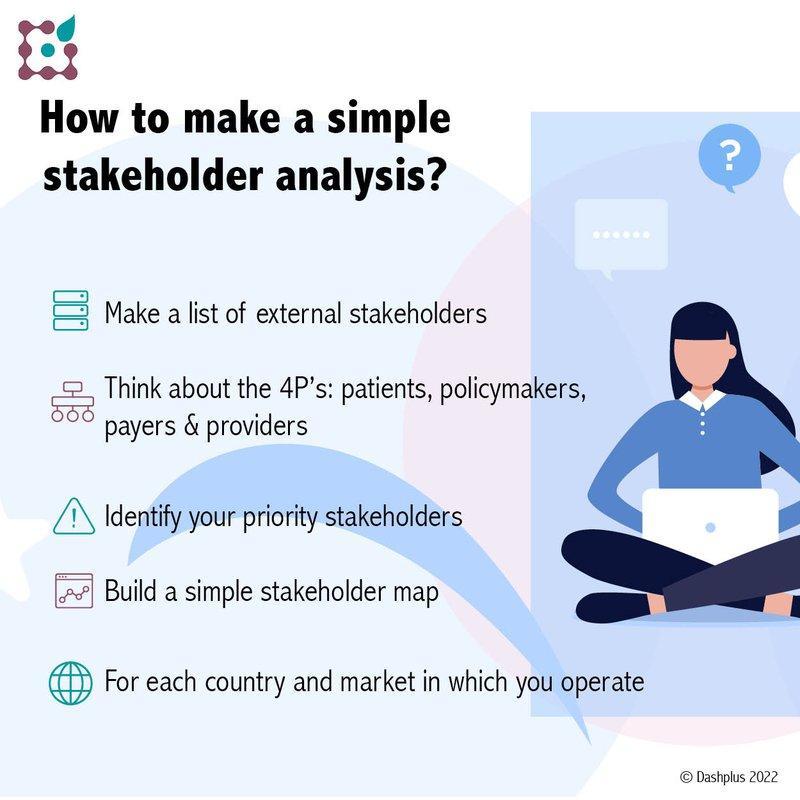
Takeway message: how to make a simple stakeholder analysis?
- Make a list of the external stakeholders involved with your product or service.
- In doing so, think about the 4 P’s: patients, policy makers, payers and providers: who is involved and/or has an interest in your project?
- Define who is a priority stakeholder: whose support is crucial to the success of your project? What player is central in your business model? What stakeholder can potentially have the largest negative impact on your growth?
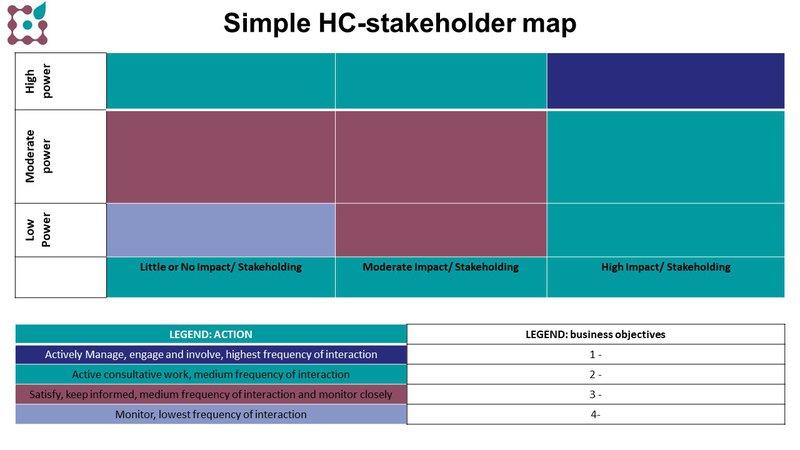
- Put your stakeholders in a simple stakeholder map (the interest grid or Mendelow matrix) like this one
- Since healthcare systems in each country are specific, repeat this excercise for each country in which you actively want to roll out your innovation.