This is the first of 3 blogs on the telehealth landscape in Portugal. The southern-European country has tackled an economic and healthcare crisis successfully last decade. No doubt, the country's early perseverance to invest in telehealth helped to bring this success.
We talked to Micaela Monteiro and Steven Braekeveldt
You may have noticed: Portugal is ‘catching up’ in the telehealth-overview we published last year (see below). And the only reason why we didn’t take the country with the frontrunners is because the infograph focused on telehealth in public primary health care: Portugal started early with telehealth in specialist care, but it wasn’t since the covid-pandemic telehealth got used in primary care too.

Portugal has been investing in telemedicine already since the mid-2000’s. For that reason, the southern-european country can safely stand alongside Finland and Sweden.
But there is more: thanks to
- the perseverance of crucial people in the healthcare system and
- a public framework open for telemedicine,
Portugal has made telemedicine a commodity. Today, public and private providers offer large hybrid care services now.
We talked to Micaela Seemann Monteiro on this topic. Dr. Monteiro is a renowned tele- & eHealth expert and experienced physician. She worked and lived in Germany and the UK before she was commissioned by the Portuguese government to establish the National Center for TeleHealth in 2016. In this position she was the driving force behind PENTS (2019). Right now, Micaela Monteiro holds the position as Chief Medical Officer for digital transformation at CUF, Portugal largest private healthcare provider.
No doubt, she is thé lady to think about when I’m referring to ‘crucial people in the healthcare system’ who have made telehealth a commodity in Portugal.’ She was and is leading in the Portuguese vision, framework and actions to stimulate telemedicine.

We also talked to Steven Breakeveldt of Ageas, who’s working on the private side of the spectrum. He’s a Belgian who has worked all over the world in leading insurance positions. Since 2010, he is CEO of Ageas Portugal. You can discover this and much more in our next blog on telehealth in Portugal.
Although public and private healthcare are separated systems in Portugal, both stakeholders are convinced telehealth helps to make healthcare sustainable by:
- tackling the problem of long waiting times in SNS (public system)
- delivering qualitative care: bringing the best and right care to the right patient
- investing in health literacy, prevention and value-based healthcare
About Portugal and its healthcare system
Portugal has a population of over 10 million inhabitants and a life expectancy of 81,1 – slightly higher than the EU average. Portugal's health spending per capita is lower than the EU average, but with the biggest share of outpatient care on the continent.
The modern Portuguese healthcare system was founded in 1979 with the formation of the Portuguese National Health Service (NHS), known as the SNS, Serviço Nacional de Saúde. In this national system, all patients (whether Portuguese citizens or expats) have access to all services. They only need to pay a small additional fee for specific services.
However, the system has its pain points:
- due to the ageing population, people are living longer (at home) and have a higher healthcare need
- Portugal has high outpatient costs: they make up 46% of the public health spending (the highest share in Europe)
- Long waiting times: due to the rigid referral system within NHS services GP’s and primary care centres (with nurses) act as strong gatekeepers to the system
- nursing workforce is lower than in other European countries
The combination of these points made it necessary, already long before the pandemic, to invest in telehealth.
And it was further encouraged for physicians and psychologists as a way to tackle the pandemic. According to Eurofound, 44% of Portuguese people reported using teleconsultation services in 2020.
- Join our Community
This is how Portugal made telehealth a commodity
3 points were crucial in the telehealth-journey of Portugal. They might inspire other countries and healthcare stakeholders too:
- Bottom-up perseverance: telemedicine implementation based on use cases and in-system experts pushing telehealth to policymakers
- A financial stimulation and open rules
- The importance of e-prescriptions to introduce new type of HC-services
Let’s take a closer look at all 3:
1. Bottom up perseverance and in-system experts pushing telehealth
Already from the 1990’s, Portugal was involved in telehealth & telemonitoring initiatives, says Micaela Seemann Monteiro. ‘Right from the start, we worked with concrete usecases where digital had already brought clear added value on a smaller scale.’
Tele-expertise in pediatric cardiology was one example. Referral from GP’s to specialists based on telehealth (so telehealth as a first contact between a patient and a specialist) was another. It aimed to diminish waiting times in public hospitals and ‘the digital before physical principle’ was even made obligatory for specialists at a certain moment. In dermatology this immediately resulted in 20-40% faster diagnosis and medical advice for patients.
It took early adoption initiatives like this and a lot of lobby work to convince politicians about the importance of making telemedicine a priority on their agenda. ‘Ever since the beginning, we wanted telehealth to be an integrated part of the normal healthcare process, not something external’.
And it took further work in hospitals, expert push and just before the pandemic: a national strategic plan (PENTS) to scale telehealth up and harmonize it across the country. Since many of the telehealth initiatives until then were local and not yet in primary care. Micaela Seemann Monteiro: “the purpose of these negotiations and of the plan, has always been to scale and improve the quality, sustainability & affordability of the system.”
It all led to the aforementioned results during the COVID-pandemic.
Portugal is leading in telehealth now.
And very interesting: SNS Portugal publishes a monthly update on telehealth consultations in a live and interactive dashboard. It learns us a lot about regions, first use versus follow-up consultations, etc.
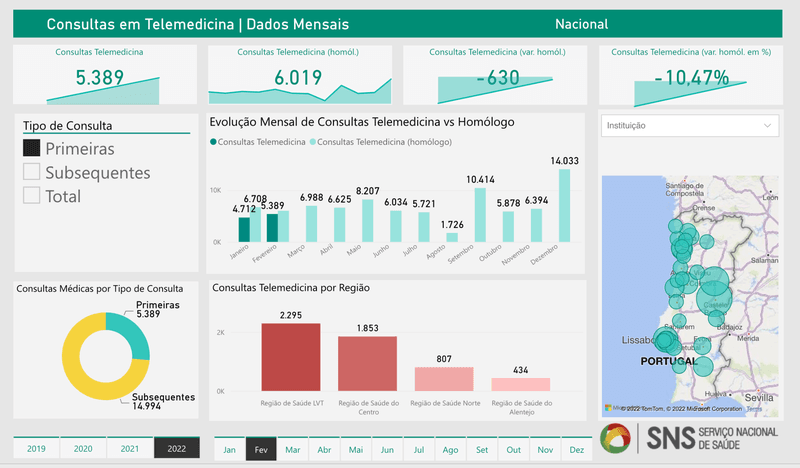
But all of this wouldn’t have been possible without a stimulating legal framework and public financing of telehealth services by healthcare professionals.
2. Financial stimulation for telehealth and open rules
Portugal started using telemedicine from 2006 on. Financing of digital consultations is similarly as to in-person healthcare. ‘In the very beginning, telemedicine sometimes was stimulated by providing higher fees for digital consultations.’
Indeed, as medical professionals are often reluctant to use telehealth on a large scale, it takes at least a similar reimbursement of digital health services as in-person services to make it work. Also other healthcare systems like Sweden have pushed towards sustainability this way.
Moreover, to make hybrid care a commodity, open rules are necessary: in Portugal there have not been specific laws or different regulations for digital HC-delivery alone. The same regulations as for in-person care apply.
But there are professional medical guidelines, training and tools for healthcare professionals, giving them support and confidence. And of course, GDPR-rules have to be followed.
Main guidelines involve:
- the GP decides whether a teleconsultation is appropriate for the specific case
- consent between doctor and patient to use a digital consultation
- specific technical guidelines by the health directorate (for teledermatology for example)
These kinds of open rules also make it possible for the system to learn and adapt to future needs.
“In the very beginning, we even stimulated the use of telemedicine by providing higher reimbursements for digital care than for physical care.”
– Micaela Seemann Monteiro
Last, but not least: Portugal has built all necessary infrastructure to make telehealth a commodity.
3. The importance of e-prescriptions to new type of HC-services
E-prescriptions are a crucial step at the end of almost any telehealth contact: if it’s not possible to receive a digital prescription (for medication, sick leave, therapy or coaching, …), it doesn’t make much sense. Nor in terms of efficiency, nor in terms of patient experience.
In general, e-prescriptions serve as a leverage for the telehealth process. Because they are crucial to ‘close the loop’ and build hybrid HC-services along the continuum: for example in primary care, pharmacies, chronic care, recovery and re-integration.
Portugal was one of the first European countries to introduce e-prescriptions. They were put into practice in hospitals ever since 2004. This is the same as in Finland. To compare: e-prescriptions started in Belgium in 2013 and in France only in 2019. Portugal is also the first, together with Finland, Estonia and Croatia, to have implemented European cross-border e-prescriptions.
Conclusion:
Portugal has made telehealth a commodity: 87% of hospitals and 44% of GP’s use telehealth consultations frequently. This is the result of :
- working with small-scale usecases
- the perseverance of in-system experts to push telehealth forwards in a no-nonsense way
- motivating fees and open framework plus general guidelines for healthcare professionals
- e-health building blocks like e-prescriptions
This way, telehealth helped to tackle the COVID-pandemic in Portugal.
But there is more: important stakeholders perceive telehealth as necessary to protect the sustainability and the quality of the healthcare system (also including its accessibility). And there’s no difference between public and private players in that regard.
Moreover, telehealth financing and the low threshold framework have:
- pushed telehealth into the system
- made it possible for private healthcare companies to develop new healthcare-services
- and for Portuguese telehealth startups to grow
Hybrid care, the seamless combination of digital care and in-person care is the next step for the Portuguese ecosystem.
What can you do next?
- Subscribe to the dashplus community to receive more insights on telehealth (it’s FREE)
- Check out how telehealth is used in other European countries
- Contact us if you want to understand how telehealth is used in your country now and what’s the impact
- Join +2000 health innovators










